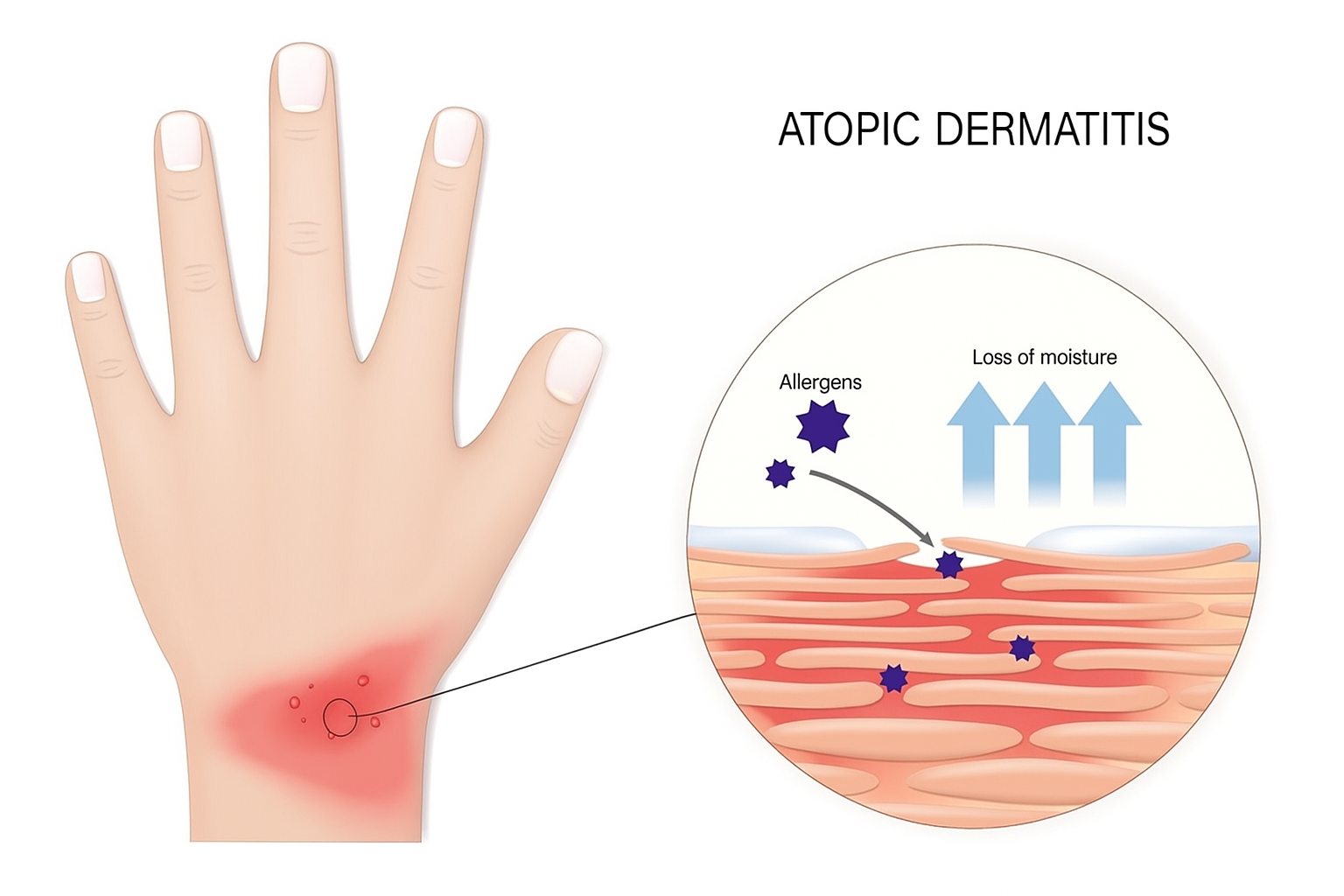
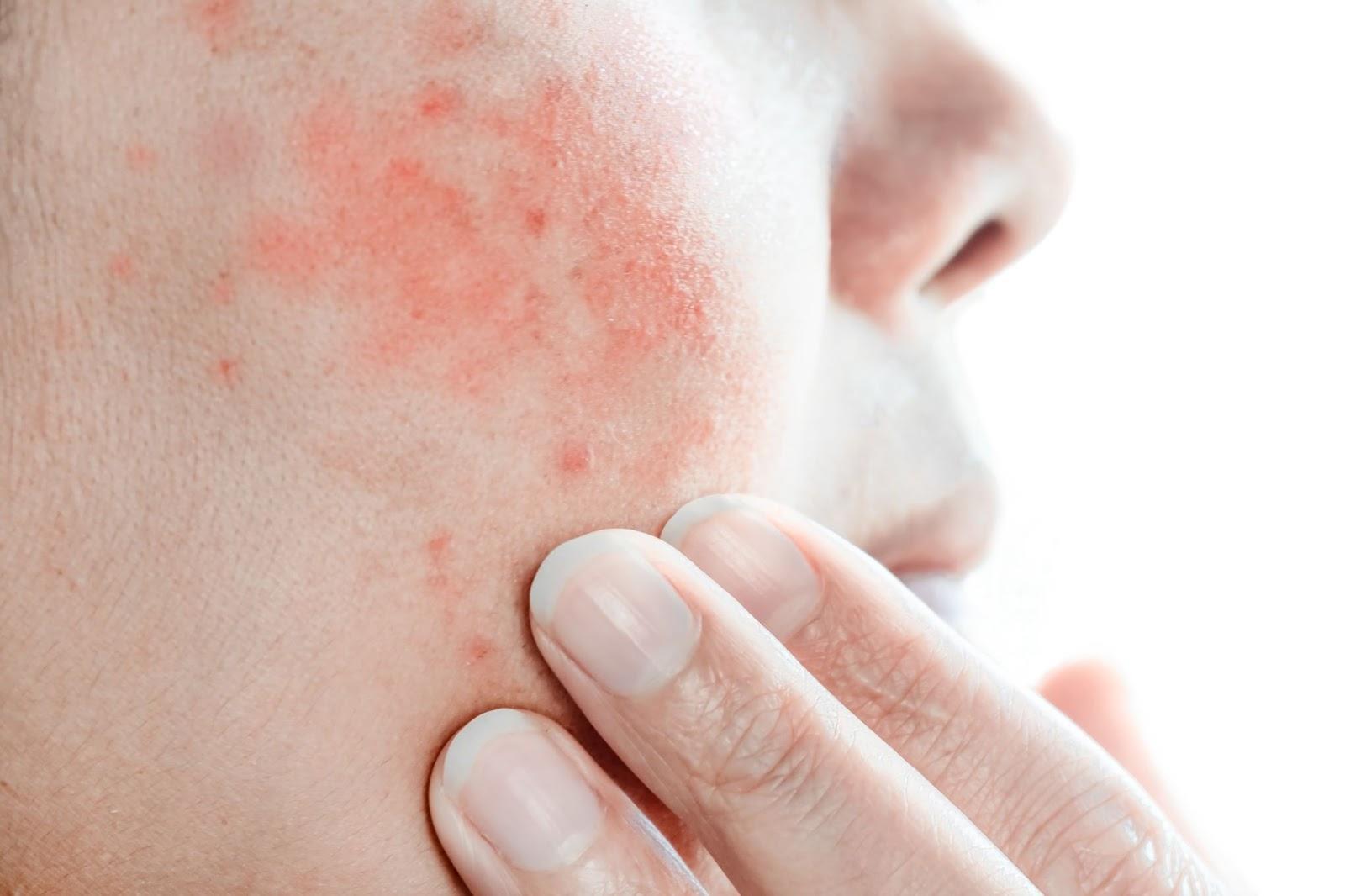
Who is at risk of Eczema in Singapore?
Although the skin condition can affect individuals across various age groups in Singapore, certain factors increase the susceptibility. This includes:
- Genetic predisposition — individuals with a family history of atopic conditions such as eczema, asthma or allergic rhinitis are more likely to develop eczema.
- Environmental triggers — the hot and humid weather, along with common allergens like dust mites and pollutants, can exacerbate eczema symptoms.
- Lifestyle factors — high stress levels, sleep deprivation, poor diet and a lack of physical activity have been associated with increased eczema severity.
- Dietary patterns — emerging research suggests that dietary patterns may influence eczema severity. Diets low in plant-based foods and high in processed or inflammatory foods could worsen symptoms in some individuals. However, more studies are needed to confirm this link in adults.
- Higher socioeconomic status — some studies have linked higher socioeconomic status with increased eczema prevalence. This is possibly due to greater use of skincare products, indoor allergen exposure or hygiene-related factors.
- Comorbid conditions — conditions like obesity, hypertension and type 2 diabetes have been associated with more severe eczema cases due to systemic inflammation.
How is Eczema diagnosed?
A detailed clinical evaluation is often the go-to diagnosis method to confirm eczema. This is because there is no single test for it. Diagnosis relies on a combination of methods, including:
- Medical history — the dermatologist will ask about the onset, duration and pattern of your skin symptoms. They may also ask about any family history of eczema, allergies, asthma or hay fever. Lifestyle habits, stress levels and exposure to irritants may also be discussed.
- Skin examination — a visual inspection helps assess the affected areas, noting their location, texture and severity. Eczema can sometimes mimic other skin conditions. Hence, a thorough assessment is important to rule out alternatives like psoriasis or fungal infections.
- Patch testing — used when a contact allergy is suspected, especially in allergic contact dermatitis. Small amounts of allergens are placed on the skin to check for delayed reactions.
- Skin swabs or biopsies — these tests may be done if there is a suspected infection or if the condition is not improving as expected. Skin swabs can check for bacteria like Staphylococcus aureus, which often worsens eczema. A skin biopsy might also be needed to rule out other skin conditions that look similar.
What are the treatment options for Eczema in Singapore?
The treatment focuses on calming inflammation, repairing the skin barrier and reducing flare-ups. Treatment approaches are tailored to the severity and type of eczema, as well as each individual’s specific triggers.
Skin barrier repair — the cornerstone of eczema management
- Moisturisers — used daily to hydrate and protect the skin.
- Soap substitutes and gentle cleansers — to avoid stripping the skin’s natural oils.
- Bath additives — like colloidal oatmeal or bath oils that soothe and moisturise.
Anti-inflammatory topical therapy — calming inflammation, redness, and itching
- Topical corticosteroids — available in different potencies for different body areas.
- Topical calcineurin inhibitors — such as tacrolimus and pimecrolimus for delicate areas or as steroid sparers.
- Topical PDE4 inhibitors — crisaborole is the only currently approved topical PDE4 inhibitor and is used to treat mild-to-moderate eczema.
Systemic treatments — for severe or unresponsive eczema
In recent years, newer targeted therapies have transformed eczema care. These medicines focus on specific pathways in the immune system, aiming to control symptoms with fewer widespread effects compared to older treatments.
This includes:
1. Biologics
Biologics are targeted treatments that work by blocking specific proteins in the immune system that drive eczema inflammation. They are designed to reduce redness, itching and skin damage by calming overactive immune responses.
These medicines are given as injections under the skin, either at home or in the clinic, usually every 2 to 4 weeks depending on the drug and the treatment plan.
Options include:
- Dupilumab — the first biologic approved for eczema. It blocks interleukin-4 and interleukin-13, two key signalling proteins involved in inflammation and itch. This treatment is suitable for children from 6 months of age in certain cases, as well as older children, adolescents, and adults.
- Lebrikizumab — targets interleukin-13, helping to improve skin barrier function and reduce symptoms.
- Nemolizumab — blocks the receptor for interleukin-31, a protein closely linked to itch signalling, making it especially promising for severe itching.
2. JAK inhibitors
Janus kinase (JAK) inhibitors are a newer class of medication that work by blocking specific immune pathways involved in eczema. They are used when eczema remains uncontrolled despite standard topical or systemic treatments.
Options include:
- Oral JAK inhibitors — such as upadacitinib and abrocitinib. These are taken daily and have shown rapid improvement in itch, inflammation and skin healing. They are suitable for adolescents and adults with widespread or persistent eczema.
- Topical JAK inhibitors — like ruxolitinib cream, they are used for localised eczema. They are particularly recommended for delicate areas such as the face or skin folds, where steroids may be less appropriate.
- Specialist monitoring required — because of possible side effects like infections or changes in blood counts or cholesterol, our dermatologist will check if the treatment suits you. They will also monitor you with regular follow-ups and blood tests.
Infection management — addressing secondary skin infections
Bacterial infections are often caused by Staphylococcus aureus, which commonly colonises eczema-affected skin and can trigger flare-ups.
- Topical antibiotics — such as fusidic acid or mupirocin, used for mild, localised infections.
- Oral antibiotics — such as flucloxacillin, prescribed for more widespread or deeper bacterial involvement.
- Antiseptic washes — including chlorhexidine or dilute bleach baths. These help reduce bacterial load and prevent recurrent infections.
Viral infections are less common but potentially serious. These can occur when eczema skin is exposed to viruses like herpes simplex.
- Eczema herpeticum — a rare but serious viral infection that appears as painful, rapidly spreading blisters.
- Oral antivirals — such as acyclovir or valacyclovir, are used to control the infection.
Phototherapy — using UV light to reduce inflammation
- Narrowband UVB phototherapy — the most common and well-tolerated method, administered in a clinical setting 2 to 3 times per week.
- PUVA (psoralen + UVA) — less commonly used, typically reserved for very severe cases.
Trigger identification and lifestyle management — reducing future flares
- Allergen and irritant avoidance — such as fragranced products, synthetic fabrics or certain foods.
- Stress management — techniques like mindfulness or counselling to reduce stress-related flares.
- Dietary review — assessing whether any foods contribute to flare-ups (though true food allergies are rare in adult eczema).