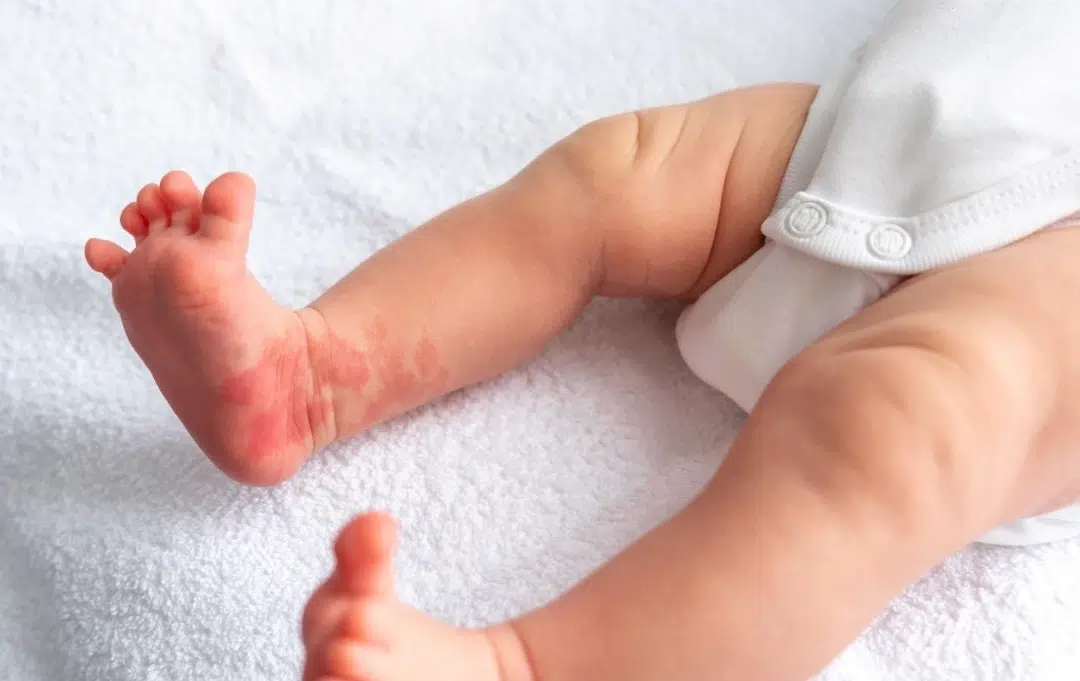
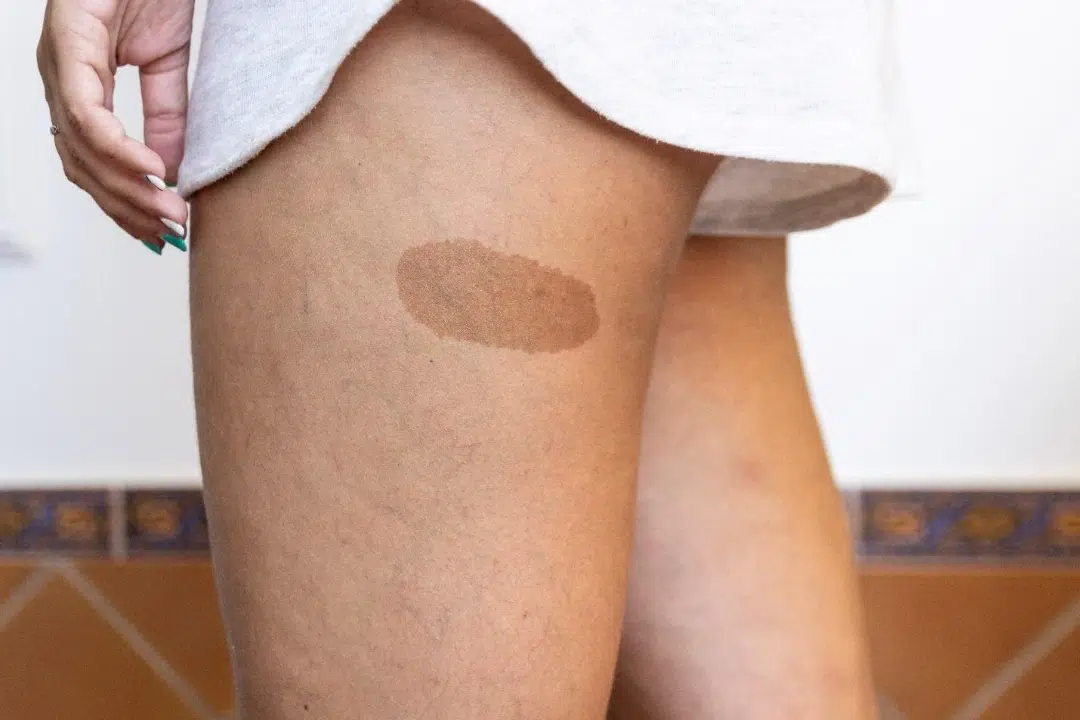
Birthmarks on the body, such as the thigh, are usually harmless and may simply be monitored as a child grows.
Do birthmarks pose any health risks?
Most are harmless and purely cosmetic. However, a small proportion may be associated with underlying medical conditions, particularly if large, rapidly growing or present in multiple areas.
This includes:
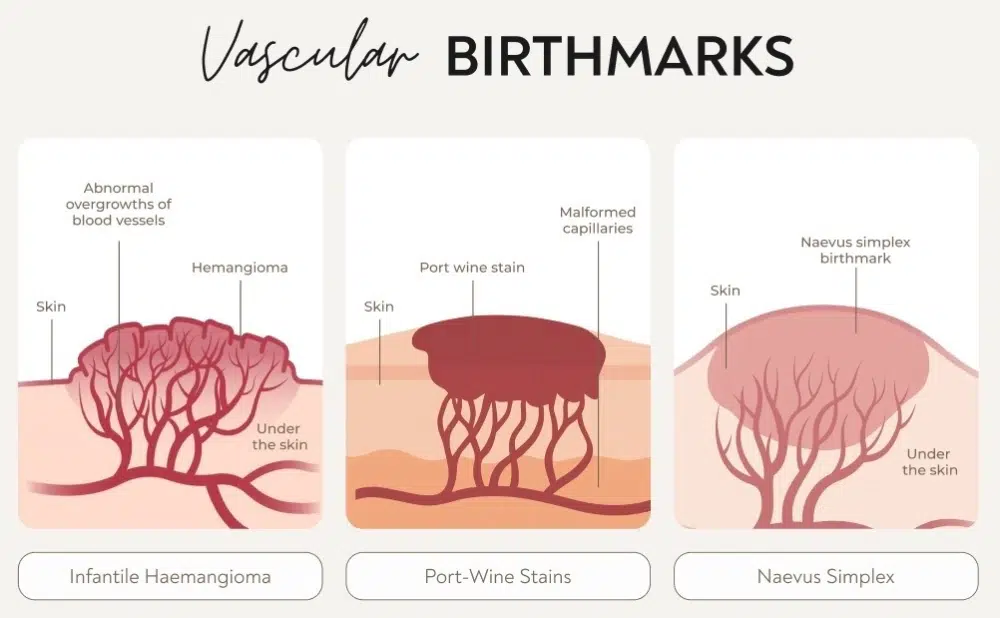
- Extensive port-wine stains may occasionally require further evaluation to rule out deeper involvement.
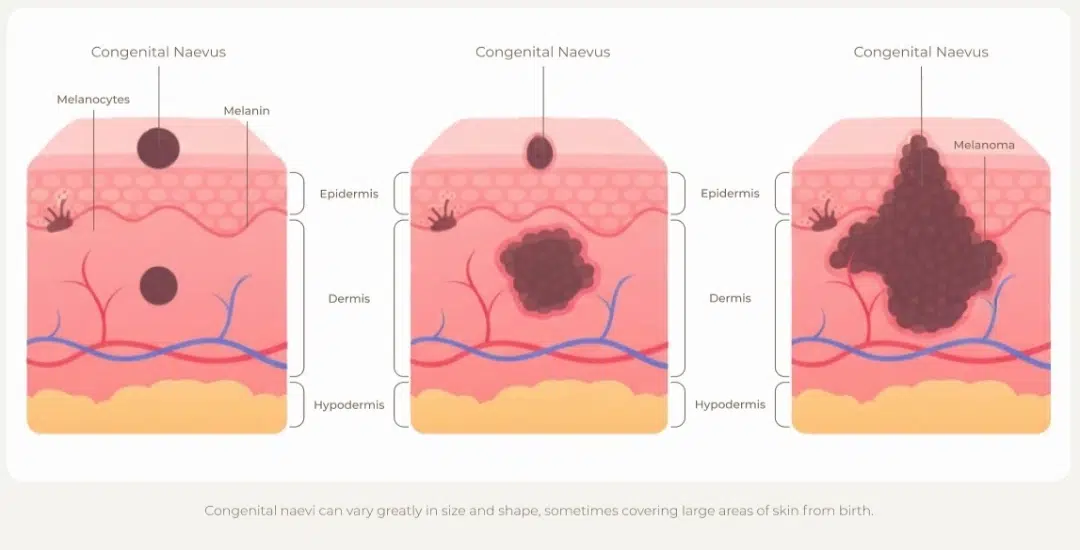
- Large congenital naevi may carry a slightly increased lifetime risk of melanoma, which is why regular dermatological monitoring is recommended.
How are birthmarks diagnosed in Singapore?
Birthmarks are usually diagnosed through a careful clinical assessment. This allows the dermatologist to determine the type of birthmark, its depth and whether any further investigations are needed.
Evaluation includes:
Clinical examination
Our dermatologist will examine the birthmark’s colour, border, texture, size, shape and location. They will also review when it appeared, either at birth or later and note any changes in growth, thickness or symptoms.
Dermoscopy
A dermoscope helps visualise fine structures within the skin. This reveals subtle differences between different lesions, allowing more precise diagnosis without the need for biopsy. Dermoscopy is particularly helpful in distinguishing between benign moles and atypical pigmentary growths.
Imaging studies
When deeper or complex vascular malformations are suspected, non-invasive imaging such as ultrasound, magnetic resonance imaging (MRI) or computed tomography (CT) angiography may be used. These techniques assess the depth of the lesion, involvement of underlying tissues and blood flow patterns.
Biopsy and laboratory tests
A skin biopsy may be performed if the birthmark has unusual features, shows rapid change or raises concern for malignancy. This involves removing a tiny tissue sample for microscopic examination. Blood tests are rarely required but may support diagnosis if a birthmark is associated with a systemic or genetic condition.
How are birthmarks treated in Singapore?
Most birthmarks are innocuous and only need observation. However, when a lesion affects appearance, function or carries a medical risk, treatment may be advised. The goal is to either reduce visibility, prevent complications or restore comfort and confidence.
At Dermatology Collective, treatment decisions are guided by the type of birthmark, its depth and the patient’s age. Modern dermatological therapies offer safe and precise options for both vascular and pigmented lesions with minimal downtime, such as:
Vascular birthmarks
- Monitoring and reassurance – many vascular birthmarks, such as infantile haemangiomas, often shrink or disappear on their own over time. Regular observation by a dermatologist helps track changes, provide reassurance and ensure intervention is only needed if complications arise.
- Pulsed Dye Laser (PDL) – the gold standard for lightening port-wine stains and persistent vascular marks. The laser targets abnormal blood vessels while sparing surrounding skin, making it safe for infants and adults alike. Early intervention often leads to better results.
- Beta-blockers (oral or topical) – commonly used for infantile haemangiomas. Medications such as propranolol slow abnormal blood vessel growth, causing the lesion to shrink and fade over time. Treatment is closely monitored for safety and effectiveness.
- Surgical removal – reserved for large or complex lesions that do not respond to medical therapy or interfere with function. Surgery aims to improve both appearance and comfort and may be performed once the lesion stabilises.
Pigmented birthmarks
- Monitoring and reassurance – many pigmented birthmarks remain stable and only require periodic review. Regular follow-up ensures stability and early detection of any concerning changes.
- Surgical excision – performed when the lesion is large, affects cosmesis or if malignancy cannot be ruled out.
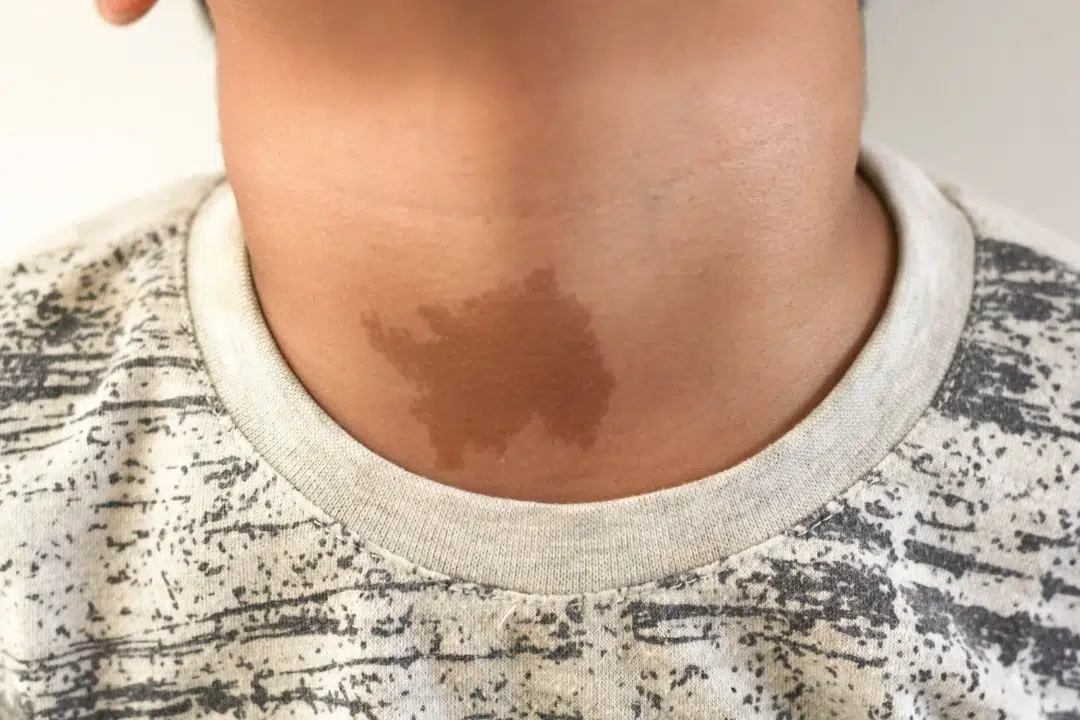
- Laser therapy – pigment-specific lasers such as the Q-switched or picosecond laser can selectively break down excess melanin in some pigmented birthmarks, e.g. café-au-lait spots.
Supportive and adjunctive care
- Sun protection – using sunscreen daily helps prevent darkening of pigmented birthmarks and protects sensitive treated skin.
- Gentle skincare – avoiding harsh scrubs and irritants helps maintain skin health, especially after laser or surgical treatments.