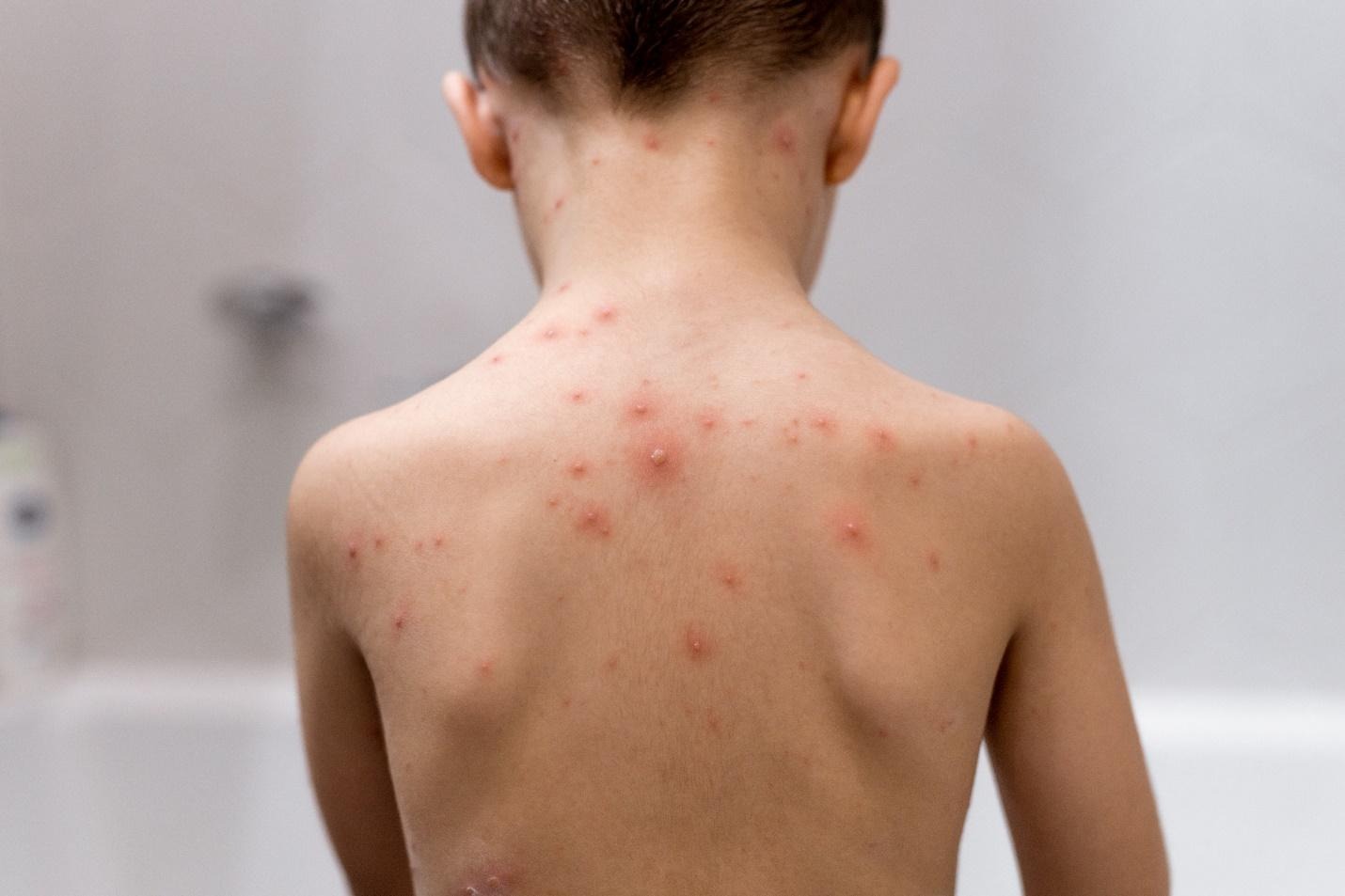
Paediatric skin infections are frequent in children due to their developing immune system and delicate skin.
Children’s skin is more delicate and their immune systems are still developing, making them more prone to infections than adults. Everyday activities, such as playing at school, running around playgrounds or attending daycare, increase exposure to germs.
Paediatric skin infections can range from mild and short-lived to more persistent conditions requiring medical treatment. Recognising the signs early and seeking prompt care not only helps your child feel more comfortable but also prevents the infection from spreading to others.
What are the types of Paediatric Skin Infections?
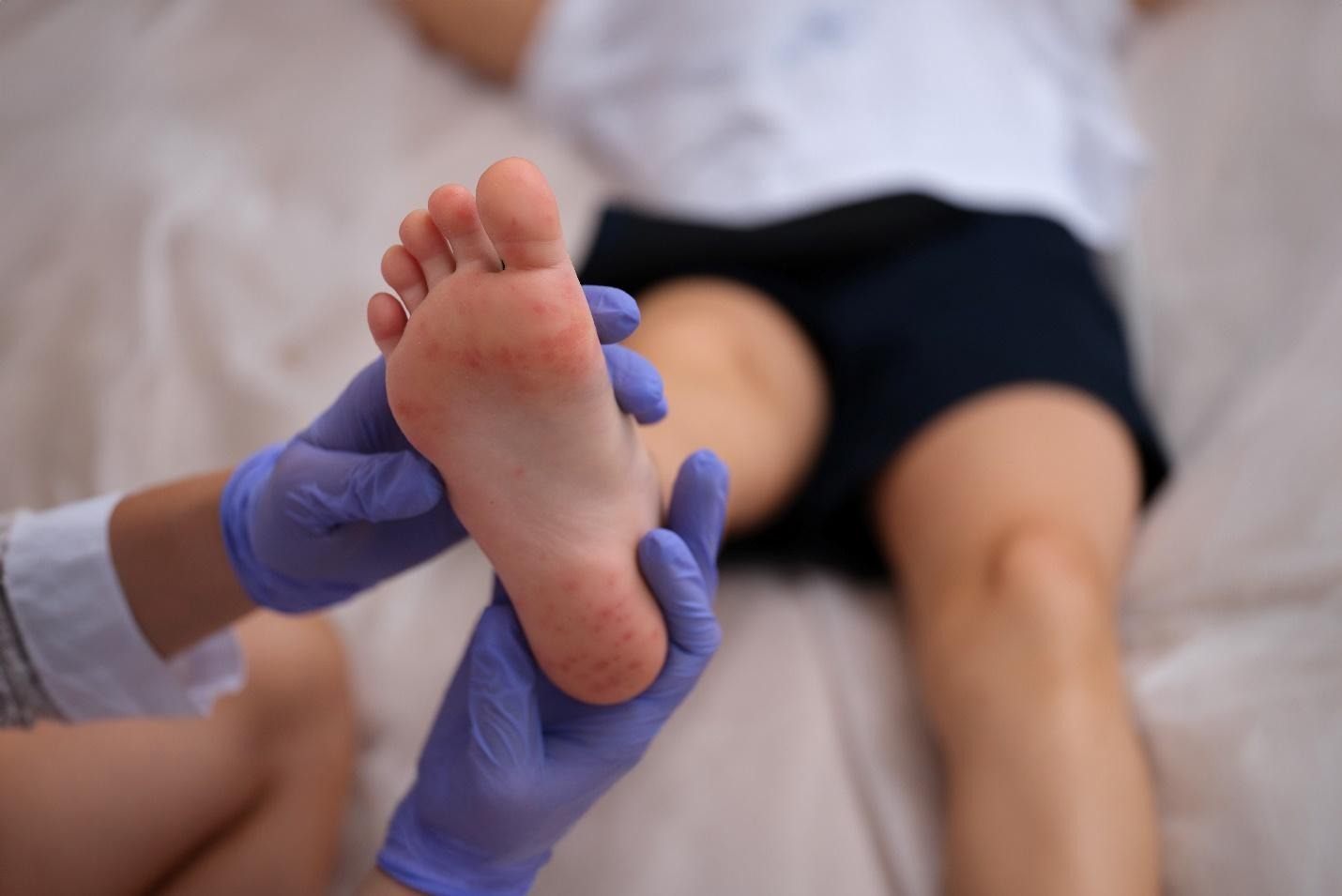
Skin infections in children are commonly caused by bacteria, viruses, fungi (including yeasts) or parasites. Each type has distinct causes, ways of spreading, appearances and common infections.
This includes:
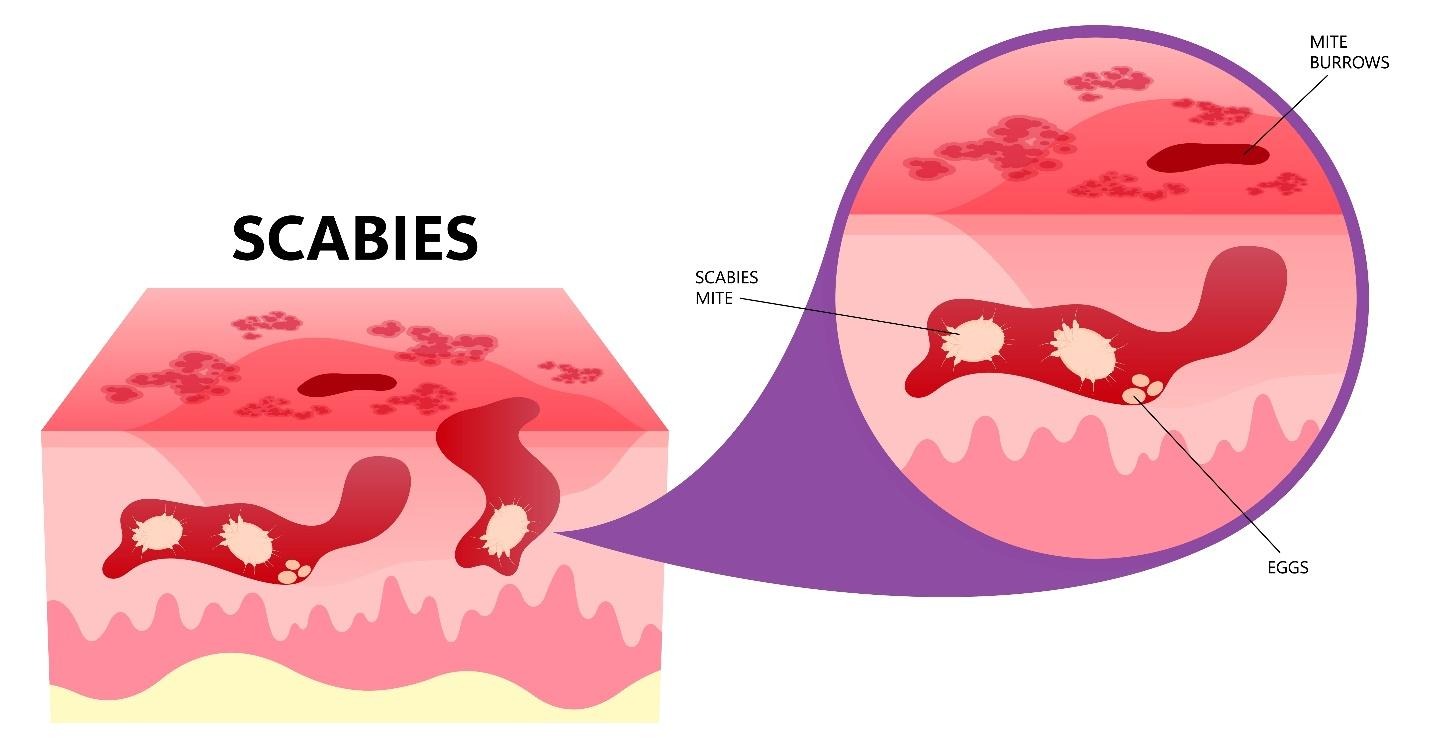
Scabies spreads easily among children through close skin-to-skin contact, shared clothing, bedding or toys.